In Healthcare, Is The Human Being An Asset Or Liability?
This article contrasts the application of preventive and predictive technologies in industry to those in healthcare. For years, risk managers have been discussing the rationing of care. This article presents the perspective of an engineering professional from the manufacturing industry who now consults with healthcare risk managers.
The human being is often referred to as an “asset” in our society. Do we actually treat people as assets or liabilities? When preventive maintenance is routinely performed on a piece of equipment, the benefits are more reliable operations, increased productivity, and lower life cycle costs. If these proactive concepts are applied to the human body within our current healthcare systems, will we see these same benefits?
Are humans assets?
The healthcare reform debate has forced a deeper look into humanity itself and its contribution to society and raises a rhetorical question:
Are humans really assets?
Merriam-Webster’s defines asset as follows:
- the property of a deceased person subject by law to the payment of his
or her debts and legacies b: the entire property of a person, association, corporation,
or estate applicable or subject to the payment of debts - an item of value owned or the items on a balance sheet showing the book value of property owned.
Merriam-Webster’s defines liability as
- the quality or state of being liable
- something for which one is liable; especially: pecuniary obligation: debt—usually used in plural
- one that acts as a disadvantage: drawback.
Experience tells us that someone who says, “Our people are our greatest assets,” is not being truthful in a literal sense. How many times do CEOs make this statement during speeches to shareholders? How many times has this kind of statement been published in the opening paragraph of annual 10K reports?
Ironically, in these reports where the CEO opens with a tribute to “our people [as] our greatest assets,” the balance sheet shows that people are listed as a liability and equipment is an asset. What is the moral perspective? Does society truly view people as assets? The debate on healthcare has challenged that premise.
Preventive And Predictive Maintenance
Those who have worked in manufacturing are familiar with the concepts of preventive and predictive maintenance (P/PM). These technologies (e.g., vibration monitor ing) can assess the condition of a piece of equipment with out stopping the equipment or the process. Application of these technologies results in overall higher operational reliability of the manufacturing process, higher-quality products (due to fewer stops and starts of the process), lower per unit costs, and thus higher margins.
After all, if a business can accurately predict which equipment will fail and estimate when it will likely do so, staff can better plan and schedule the needed repair in a cost-effective manner. Under these conditions, they do not unexpectedly interrupt operations and can ensure the least amount of time to make the repair. In the manufacturing industry, this is called mean time to repair, which can be defined as a measure of the average maintenance performance, obtained by dividing the cumulative time for a number of consecutive repairs on a given repairable item by the cumulative number of failures of the item. The term repair means the time the defect was reported to the time the equipment was ready to restart and operate satisfactorily.(1)
Waiting For Failure To Occur
The alternative to this proactive approach is to wait for the failure to occur unexpectedly. When this happens, the impact on production is adverse (the operation is down for a longer period of time) and the repairs take longer because the appropriate people have to be assembled to perform the repair; they also must have the materials available to make the repair.
The result of the proactive approach of preventive and predictive maintenance is that the equipment (the asset) is more reliable and productive and lasts longer, increasing its value for the money originally invested for its purchase and maintenance. In industry this is referred to as life cycle costing. It takes into account not only the original purchase cost but also the cost to maintain the equipment properly over its expected lifetime.
Contrast this with the healthcare debate. Start with the understanding that equipment and people are very different in almost all respects but are treated in a similar way. People, unlike equipment, are unique: no two are the same. While two people may be diagnosed with the same disease, how they respond to treatments may vastly differ. Two people who live the exact same lifestyle may not exhibit the same diseases in their lifetime because they are genetically different and predisposed to certain diseases. For this reason, there are no canned solutions for each human as there would be for similar equipment in similar service that fails for the same reason.
When patients come to a hospital, the services they will require are not often known ahead of time, and their medical history may be vague at best. Compare this with a manufacturing plant, where specifications are available for each piece of equipment, and the product being processed is well known. A hospital does not have this luxury with patients who come to the emergency department (ED). They do not know who or how many patients are coming, at what time, and in what condition.
Similarities In Processes
In spite of these distinct differences between manufacturing and healthcare environments, their overall processes also show similarities.
The product of a hospital is the maintenance and lengthening of productive life as well as the enhancement of the quality of life for its human patient. Raw material is to a manufacturing plant what a patient is to a hospital. A manufacturing plant processes the raw material using various types of equipment and produces some type of finished product. A hospital processes a patient with an illness or someone who exhibits certain symptoms; the hospital may not know when the patient presents why these symptoms exist. The hospital as a system is focused on diagnosing and treating the illness or symptoms. This description, which may be couched in macroterms, points out the similarities in and differences between the two systems.
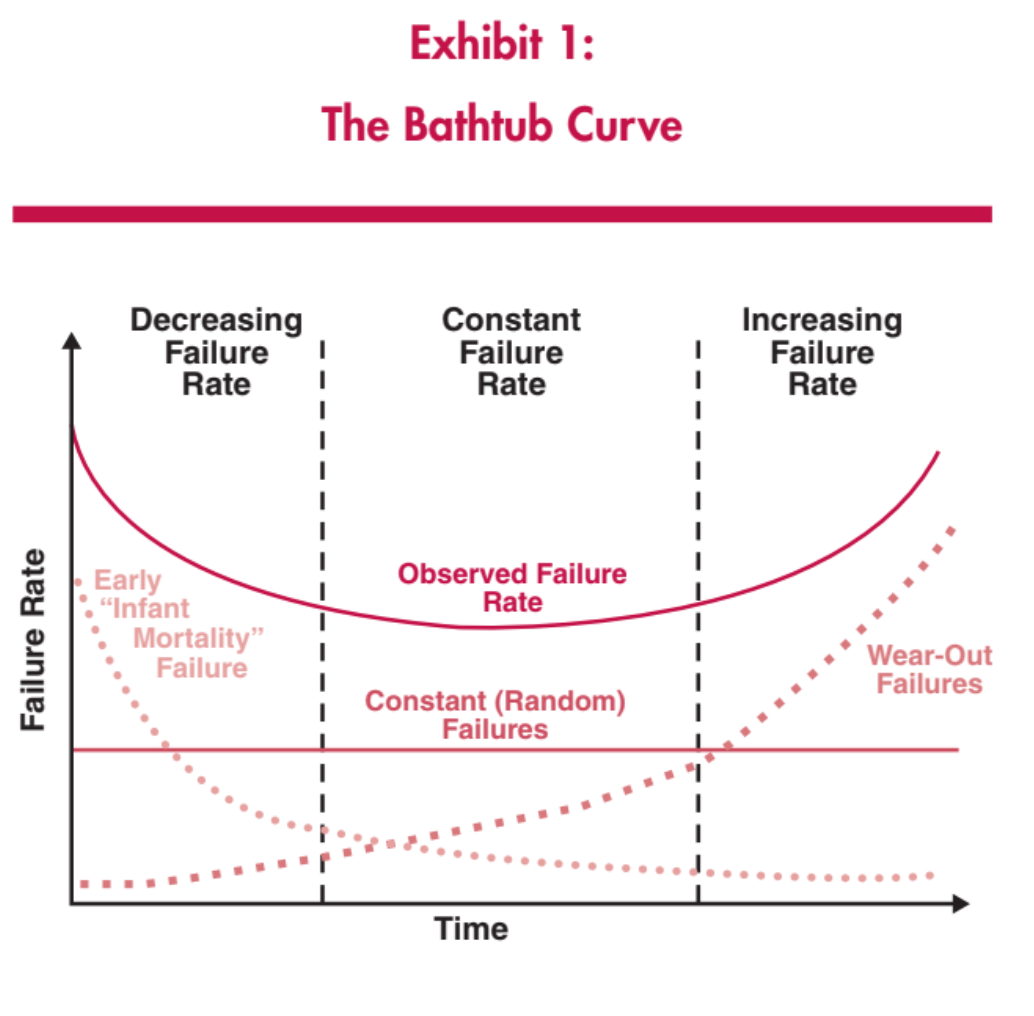
The bathtub curve (Exhibit 1) reflects similarities between equipment and humans as well. The curve is a commonly used conditional probability curve that represents the age–reliability relationship of certain items, characterized by an infant mortality region, a region of relatively constant hazard rate, and an identifiable wear-out region.(2)
In the early life of a product, according to the bathtub curve, the failure rate is high but rapidly decreases as defective products are identified and discarded and early sources of potential failure (such as handling and installation error, generally quality-related issues) are overcome. In the middle of the life cycle of a product—generally once it reaches consumers—the failure rate is low and constant. This is often referred to as the built-in failure rate. In the late life cycle of the product, the failure rate increases as age and wear take their toll on the product.
When this curve is overlaid on a human being’s lifetime, it is equally applicable. In the early stages of life, one experiences “infant mortality failures”: illnesses prone to occur in children as the human body adapts to its new environment and the growth process. Over the person’s lifetime, these failures start to become predictable from a health standpoint. For example, most adults suffer from seasonal allergies, the usual coughs and colds, and occasionally the flu. These types of chronic illnesses become expected and accepted as part of the annual routine. As they age, bodies require more servicing (i.e., more frequent monitoring and testing).
So the question at hand is whether all sides in the healthcare debate are regarding the human being as an asset and therefore acknowledging that the first and last decades of life (or periods of life) will not be as productive as the “constant period.”
Applying Principles of Preventive and Predictive Technologies To Healthcare
What would the result be of applying the principles of preventive and predictive technologies to patients as part of overall healthcare reform? These technologies in healthcare certainly exist today in the form of CT scans, MRIs, X-rays, and an array of other diagnostic and imaging technologies. These technologies allow the condition of the human body to be assessed without shutting it down. Currently one may get blood tests annually during a physical, a colonoscopy after age 50, dental checkups annually, and eye exams every six months while the body’s physiological processes continue.
People do the same thing with cars when they change the oil every 3,000 miles and the transmission fluid every 30,000 or so miles. These acts of “maintenance” are similar to the preventive and predictive tools for rotating stationary equipment in a manufacturing plant. What would be the result of applying these proactive concepts to healthcare across the board?
The initial costs would be extremely high due to the proposed number of new insureds (perhaps as many as 47 million) enrolled in insurance plans, added to the costs of accommodating the current enrollees in their respective insurance plans. While many of these new insureds are already using the ED as their entry point to the healthcare system without insurance, the preventive care described is currently not readily available to them as a result of their uninsured status. In addition, the potential cost to quality of care must be factored in as a flood of new patients enters an existing hospital infrastructure that is already lean and short-staffed. When added to the large numbers of aging baby boomers seeking services, there could well be a recipe for a quality nightmare in the healthcare system.
Many believe that complex systems would be fine if it were not for the erratic behavior of some unreliable people, often referred to as the bad apple theory.(3) However, the new view of human error sees such quality-related failures not as the fault of individuals but as the result of poor systems and their effect on the decision making of the human beings working within. When a complex system is stressed, any gaps are exposed and will contribute to poor decision making at a time when precision is needed most.
Currently patients typically get MRIs only when symptoms arise to require such technology to identify the particular problem. Similarly patients do not go to a surgeon annually and say, “Go ahead and cut me open, and see what you find. While you are in there, just fix what needs fixing.” They do not do this because, as the bathtub curve indicates, of the increased chance of human error in the infant mortality phase of the curve. This means that if surgeons do not have to go into the human body, they should not because there is a higher likelihood of human error and the overall risks outweigh the potential benefits.
Overusing Prevention
In the past when physicians attempted to apply P/PM concepts, many overused them, believing that more testing would prevent lawsuits. This choice raised healthcare costs for the wrong reasons and put such P/PM concepts out of favor because they were abused. The overuse of these types of diagnostic tests should take into consideration such technical factors as patient overexposure to radiation. Just as within industry, no one is advocating that these tests be implemented annually across the board in a generic and constant fashion.
In manufacturing, tools such as reliability-centered maintenance (RCM) techniques are designed to prioritize the criticality of equipment and their components to the overall ability to operate at full capacity at each different manufacturing facility. RCM is defined as a disciplined logic or methodology used to identify preventive maintenance tasks to realize the inherent reliability of equipment at a minimum expenditure of resources.(4) Based on that quantifiable criticality, appropriate frequency of testing is put in place. This means that the more critical the equipment may be to the operation, the more frequently it is checked when compared to the less critical.
The same methodology can be envisioned for the healthcare setting. The organs and functions of the body that are more critical to the ability to function productively would be tested more frequently than the less critical organs and functions.
Toward A More Productive Life
The upfront costs of rolling out such proactive approaches nationwide would be staggering. However, if one looks at the life cycle of human beings and the increased productivity that could be achieved with “preventive maintenance” during the extended life period, we might expect to see fewer unexpected, catastrophic illnesses.
In 2004 the elderly, who account for 12% of the population, used 34% of Centers for Medicare & Medicaid Services (CMS) expenditures.(5) In a proactive healthcare lifestyle, this would prove to be an investment in extended human productivity. People would live longer and be more productive during that extended period: they would use their skills, innovation, knowledge, creativity, and intellectual capital more fully; absenteeism would fall; and they would have increased productivity per hour. Of course, the generally accepted accounting principles cannot capture such soft costs, so it is difficult to quantify such important metrics for the finance people.
Relating this to the bathtub curve, the proactive approach would extend the steady-state or random-failure period of life (phase 2) and would also lower the curve at that point to reflect fewer failures (illnesses) and better quality of life. The costs per year of life would then be lower due to amortizing them over a long life span and encountering lower healthcare costs due to employing proactive healthcare practices.
Over the long term, there would not be as many significant costs related to treating these unexpected catastrophic illnesses and diseases. All of the associated ongoing costs would be for increased quality of life (e.g., rehabilitation, ongoing medications, at-home care, long-term care).
As a practical example, consider one of the CMS Never Events: stages 3 and 4 decubitus ulcers (DU) not present on admission (NPOA), that is, bedsores or pressure ulcers.
The average cost nationally to treat these ulcers is reported to be around $50,976 each.(6) The most recent prevalence study found that 10.8% (standard deviation 5.84) of the hospitalized patients at a given time are afflicted with bedsores.(7) Several preventive measures and protocols can economically be put in place to prevent these ulcers from occurring in the first place,(8) but these protocols have not been vigorously pursued in the past because until recently, associated costs for decubiti care have been reimbursed by CMS.
This has not been the case since October 2008, and when such an event occurs, the hospital bears the costs of treatment.(9) Of course, the most important factor that sometimes gets overlooked is that if the ulcer could be prevented, the patient would not have to endure the extreme pain and suffering associated with ulcers. This is the real cost that is never calculated in dollars but surfaces in human pain and suffering.
Longer Life Economically Feasible?
The end result here is that if invoking the proaction paradigm is aggressively pursued across the U.S. healthcare system, it could increase the length of productive human life. From a financial and a moral standpoint, is that what is being sought? Should it be? Those just interested in enjoying their short time on earth would likely be offended by someone even asking about whether the effects of lengthening life were economically feasible.
If humans (liabilities) were to be provided the courtesy that equipment (assets) is provided in manufacturing processes where reliability engineering principles are applied, they would be entitled to proactive treatment (preventive maintenance) in order to ensure they were productive for longer periods of time with fewer unexpected illnesses (failures).
From a strictly fiscal standpoint, applying the reliability principle of proaction would present a staggering
upfront cost, while the average annual life cycle cost per patient would be less for each year that the patient’s life was extended (using average life span as the benchmark). Also, each additional year longer that the patient lived would also extend the number of productive and quality years of life (versus being in decline during the same period if not living a proactive lifestyle). This is because the upfront costs are amortized over more years of life.
However, if viewed from the reactive perspective, the healthcare system will continue to treat illnesses and
symptoms as they occur and patients will die at the current average life span or earlier. When a “reactive” patient dies, all costs associated with treating that person end. During the person’s decline, he or she is not as productive to society in the literal sense.
Also, end-of-life costs are generally higher for “reactive” patients because they have more critical illnesses, which require more expensive interventions. If they live another 10 years, they are actually more expensive to the healthcare system.
CONCLUSION
From the moral standpoint, the argument is, “Should the healthcare system do whatever it takes to increase the length and quality of productive human life?”
Analogies have been made contrasting equipment to human life and the manner in which they are maintained. In the end, would applying the preventive and predictive approaches described in this article be applicable, morally acceptable, and fiscally responsible?
From a financial standpoint, extending human life (proaction) costs society more overall during a human life span even though the costs per year of life would likely be lower. Contrast this to the reactive healthcare approach or paradigm: “If it ain’t broke, don’t fix it.” The reactive approach would likely cost less over the human life span because length of life would not be maximized. Does this additional investment in the extension of human life provide increased value to society?
This becomes the dilemma in the big picture of life as finding an acceptable middle ground is debated. All parties have a vested and personal interest in this debate and should work together to arrive at a consensus. This can occur only if perspectives are voiced constructively.
Definitions
Bad apple theory: Complex systems would be fine if it were not for the erratic behavior of some unreliable people (bad apples).(4)
Mean time to repair (MTTR): A measure of the average maintenance performance, obtained by dividing the cumulative time for a number of consecutive repairs on a given repairable items by the cumulative number of failures of the item. The term restore means the time the defect was reported to the time the equipment was ready to restart and operate satisfactorily.(11)
Reliability: The characteristic of an item expressed by the probability that it will perform a required function under a stated condition for a stated period of time.(2)
Bathtub curve: A conditional probability curve representing the age-reliability relationship of certain items, characterized by an infant mortality region, a region of relatively constant hazard rate, and an identifiable wear-out region.(2)
References:
1. Narayan V, Wardhaugh, JW, Das, M. 100 Years in Maintenance and Reliability: Practical Lessons from Three Lifetimes at Process Plants. New York: Industrial Press; 2007.
2. Anderson RT, Neri L. Reliability Center Maintenance: Management and Engineering Methods. New York: Elsevier Science Publishers; 1990.
3. Latino M. Utilizing advanced statistical reliability methods to improve overall asset performance. ReliabilityWeb Article Knowledge Base. www.relaiabilityweb.com. Accessed August 22, 2009.
4. Dekker S. The Field Guide to Understanding Human Error. Hampshire, England: Ashgate Publishing; 2006.
5. Anderson RT, Neri L. Reliability Center Maintenance: Management and Engineering Methods. New York: Elsevier Science Publishers; 1990.
6. Hartman M, Catlin A, Lassman D, Cylus J, Heffler S. “U.S. Health Spending By Age, Selected Years Through 2004,” Health Affairs, 27, no. 1 (2008): w1-w12. http://www.cms.hhs.gov/NationalHealthExpendData/downloads/2004-highlights.pdf.
7. Cost Savings Through Bedsore Avoidance. National Decubitus Ulcer Foundation, Oakton, VA. http://www.decubitus.org/. Accessed September 15, 2009.
8. Barczak CA, Barnett RL, Childs EJ, Bosley LM. Fourth National Pressure Ulcer Prevalence Survey. Adv Wound Care. 1997 Jul-Aug;10(4):18–26.
9. Xakellis GC, Frantz R, Lewis A. Cost of Pressure Ulcer Prevention in Long Term Care. Am Geriatric Society, 1995 May;43(5):496–501.
10. Dekker S. The Field Guide to Understanding Human Error. Hampshire, England: Ashgate Publishing; 2006.
11. Narayan V, Wardhaugh, JW, Das, M. 100 Years in Maintenance and Reliability: Practical Lessons from Three Lifetimes at Process Plants. New York: Industrial Press; 2007.
12. Anderson RT, Neri L. Reliability Center Maintenance: Management and Engineering Methods. New York: Elsevier Science Publishers; 1990.
13. Ibid.
Attribution:
This article was originally published in 2010 in The Journal of Healthcare Risk Management • VOLUME 29, NUMBER 3
About the Author
Robert (Bob) J. Latino is former CEO of Reliability Center, Inc. a company that helps teams and companies do RCAs with excellence. Bob has been facilitating RCA and FMEA analyses with his clientele around the world for over 35 years and has taught over 10,000 students in the PROACT® methodology.
Bob is co-author of numerous articles and has led seminars and workshops on FMEA, Opportunity Analysis and RCA, as well as co-designer of the award winning PROACT® Investigation Management Software solution. He has authored or co-authored six (6) books related to RCA and Reliability in both manufacturing and in healthcare and is a frequent speaker on the topic at domestic and international trade conferences.
Bob has applied the PROACT® methodology to a diverse set of problems and industries, including a published paper in the field of Counter Terrorism entitled, “The Application of PROACT® RCA to Terrorism/Counter Terrorism Related Events.”
Recent Posts
5 Root Cause Analysis Examples That Shed Light on Complex Issues
Root Cause Analysis with 5 Whys Technique (With Examples)
What Is Fault Tree Analysis (FTA)? Definition & Examples
Guide to Failure Mode and Effects Analysis (FMEA)
Tags
Root Cause Analysis Software
Our RCA software mobilizes your team to complete standardized RCA’s while giving you the enterprise-wide data you need to increase asset performance and keep your team safe.
Get Free Team Trial
Root Cause Analysis Training
Your team needs a common methodology and plan to execute effective RCA's. With both in-person and on-demand options, our expert trainers will align and equip your team to complete RCA's better and faster.
View RCA Courses
Reliability's root cause analysis training and RCA software can quickly help your team capture ROI, increase asset uptime, and ensure safety.
Contact us for more information:

